ICSI Unit
What is ICSI UNIT ? How we can help?
Intracytoplasmic sperm injection
This procedure is most commonly used to overcome male infertility problems, although it may also be used where eggs cannot easily be penetrated by sperm, and occasionally in addition to sperm donation.
It can be used in teratozoospermia, because once the egg is fertilized, abnormal sperm morphology does not appear to influence blastocyst development or blastocyst morphology.Even with severe teratozoospermia, microscopy
Procedure
ICSI is generally performed in addition an in vitro fertilisation procedure to extract often several oocytes from a woman. The procedure is done under a microscope using multiple micromanipulation devices (micromanipulator, microinjectors and micropipettes). A holding pipette stabilizes the mature oocyte with gentle suction applied by a microinjector. From the opposite side a thin, hollow glass micropipette is used to collect a single sperm, having immobilised it by cutting its tail with the point of the micropipette.
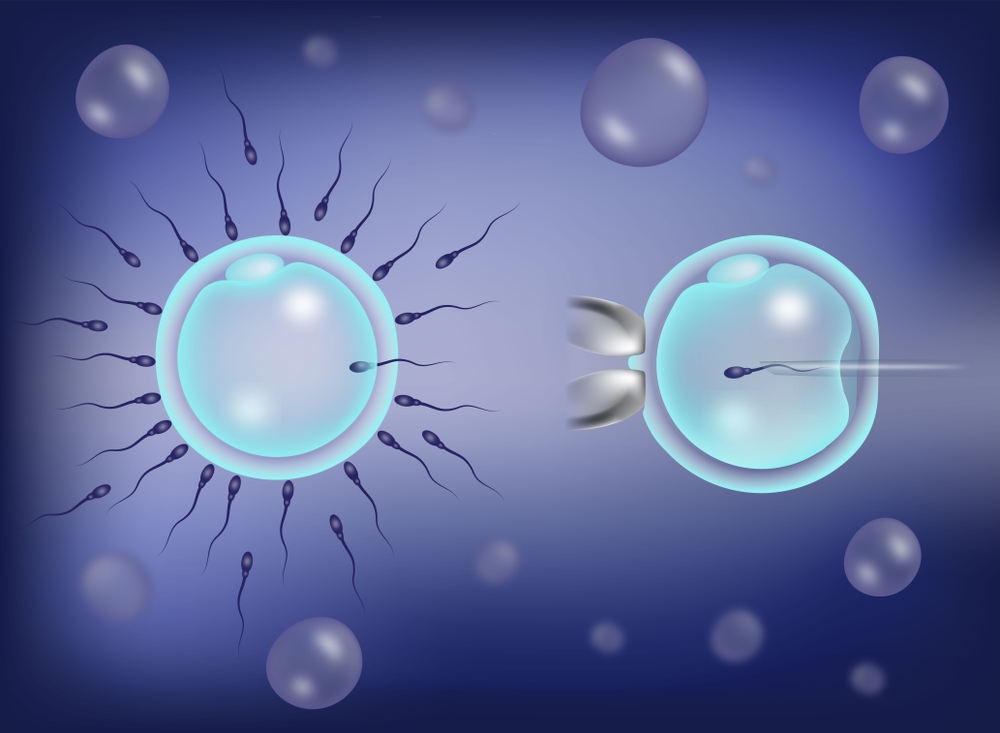
The oocyte is pierced through the oolemma and into the inner part of the oocyte (cytoplasm). The sperm is then released into the oocyte. The pictured oocyte has an extruded polar body at about 12 o’clock indicating its maturity. After the procedure, the oocyte will be placed into cell culture and checked on the following day for signs of fertilization. In contrast, in natural fertilization sperm compete and when the first sperm penetrates the oolemma, the oolemma hardens to block the entry of any other sperm. Concern has been raised that in ICSI this sperm selection process is bypassed and the sperm is selected by the embryologist without any specific testing.
However, in mid 2006 the FDA cleared a device that allows embryologists to select mature sperm for ICSI based on sperm binding to hyaluronan, the main constituent of the gel layer (cumulus oophorus) surrounding the oocyte. The device provides microscopic droplets of hyaluronan hydrogel attached to the culture dish. The embryologist places the prepared sperm on the microdot, selects and captures sperm that bind to the dot. Basic research on the maturation of sperm shows that hyaluronan-binding sperm are more mature and show fewer DNA strand breaks and significantly lower levels of aneuploidy than the sperm population from which they were selected.
A brand name for one such sperm selection device is PICSI. ‘Washed’ or ‘unwashed’ sperm may be used in the process.
Please contact us today and we’ll be happy to provide a free quote.
Intra Cytoplasmic sperm Injection (ICSI)
Intra Cytoplasmic Sperm Injection (ICSI) is the most successful micromanipulation technique, most commonly used for the treatment of male factor infertility. This technique is used to enhance the fertilization phase of in-vitro fertilization (IVF) by mechanically inserting a normal, live single spermatozoon directly into the cytoplasm of an oocyte. The fertilized egg is then placed in a woman’s uterus or fallopian tube after three or five days. The indication for ICSI :
- Severe male factor infertility such as Oligospermia and Azoospermia
- Severe endometriosis
- Polycystic ovarian diseases which do not respond to conventional treatments
- Unexplained infertility
- Previous failed IVF cycles
- multiple miscarriage
Please contact us today and we’ll be happy to provide a free quote.
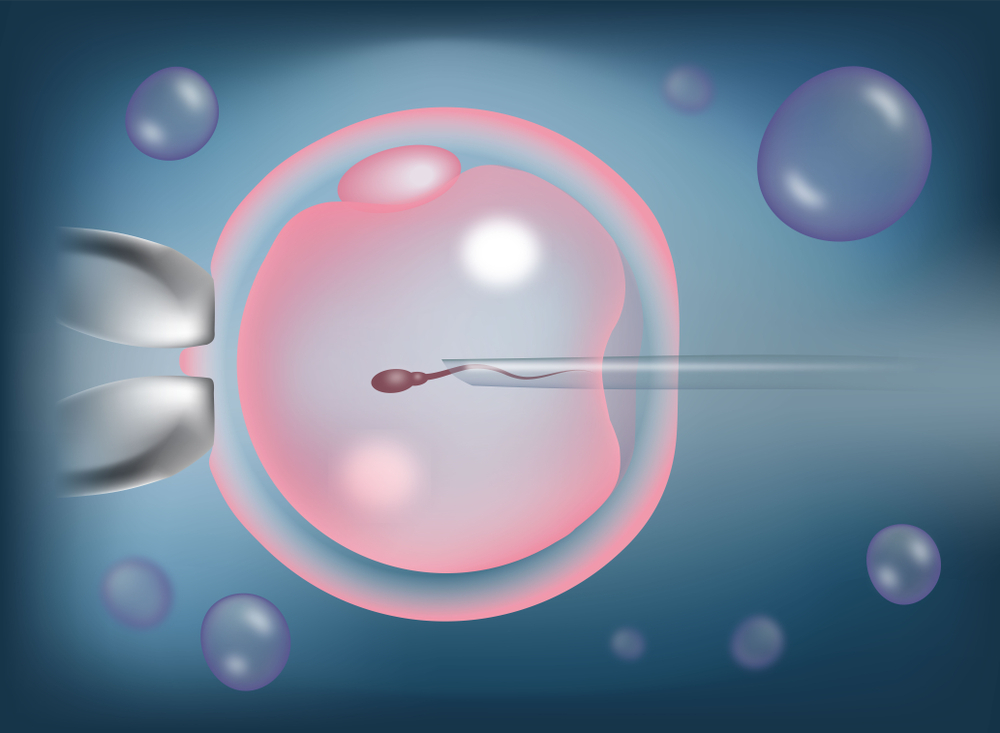
A sharp and delicate needle is used to immobilise & pick up a sperm and it is injected into the cytoplasm of the egg, after which the needle is removed. The success rate of ICSI is significantly higher than IVF and the couples often opt for ICSI when the conventional IVF technique does not produce desired results for them. The success rate of ICSI is directly proportional to the age: the younger the patient is; the higher are the chances of success.
Google Reviews
Please contact us today and we’ll be happy to provide a free quote.

